Healthcare clinicians prescribe 15 times more anti-diabetes medications than they do anti-obesity drugs, missing an important opportunity to control both diseases, researchers reported.
Their article, “Low adoption of weight loss medications: A comparison of prescribing patterns of antiobesity pharmacotherapies and SGLT2s,” was published in the September issue of Obesity, the scientific journal of The Obesity Society.
Obesity is a well-known risk factor for developing diabetes. However, although a vast proportion of people with type 2 diabetes are obese or overweight, preventive measures regarding weight gain do seem to be used fully.
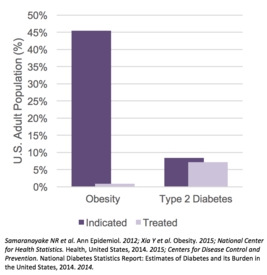
Six anti-obesity medications are now approved by the U.S. Food and Drug Administration (FDA) as treatment in combination with a reduced-calorie diet and increased physical activity. But the research found that only 2% of the potential 46% of eligible adults in the U.S. receive these drugs.
“Obesity is a serious disease that is not getting serious treatment,” Charles Billington, MD, FTOS, past president and spokesman for The Obesity Society, said in a press release. “We are missing the opportunity among patients with serious obesity-related illness to provide the full range of proven, safe and effective therapies. It’s time to start treating people with obesity as we would others with chronic diseases — with compassion and access to evidence-based care in a clinical setting.”
“Given the close tie between obesity and type 2 diabetes, treating obesity should be an obvious first step for healthcare providers to prevent and treat diabetes. By treating obesity, we may be able to decrease the number of patients with type 2 diabetes, among other related diseases and the medications used to treat them,” said Catherine E. Thomas, MS, the Weill Medical College of Cornell University researcher who led the study. “A greater urgency in the treatment of obesity – on the part of clinicians and patients – is essential. We’re talking about prolonged and better quality of life for patients.”
Thomas and her team analyzed data, dating from 2012 to 2015 and taken from two different databases, to examine prescription trends for anti-diabetes and anti-obesity medications. According to the researchers, the prescribed amount of anti-diabetes drugs, not including insulin, was 15 times higher than that of anti-obesity drugs. The majority of these prescriptions was found to be given by general practitioners, family doctors, internal medicine clinicians, as well as endocrinologists.
Further barriers to obesity treatment included a lack of reimbursement for healthcare providers, limited time during office visits, lack of training in obesity counseling, and competing demands.
In a commentary that accompanied the study, “Low utilization of obesity medications: What are the implications for clinical care?” Ted Kyle, founder of ConscienHealth, said, “By comparing the adoption rate of new anti-obesity medications to the considerably faster rate for new diabetes medications, this new research provides an important snapshot of the problem.”
Kyle added that research should now focus on understanding the exact benefit of obesity medications, as measured by patient outcomes in real clinical settings, and to identifying systematic barriers in the use of such medications.


