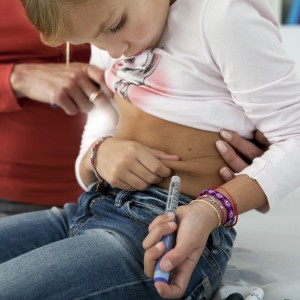
 A team led by researchers at Children’s Hospital of Philadelphia revealed that racial/ethnic differences among children with type 1 diabetes can influence the management and outcome of the disorder. The study was published in the journal Pediatrics and is entitled “Racial-Ethnic Disparities in Management and Outcomes Among Children With Type 1 Diabetes.”
A team led by researchers at Children’s Hospital of Philadelphia revealed that racial/ethnic differences among children with type 1 diabetes can influence the management and outcome of the disorder. The study was published in the journal Pediatrics and is entitled “Racial-Ethnic Disparities in Management and Outcomes Among Children With Type 1 Diabetes.”
It has been previously suggested that racial/ethnic differences in diabetes patients can influence the disease outcome. According to the American Diabetes Association, individuals from certain ethnic groups are more likely to develop diabetes. However, it is still controversial whether these differences are the result of different individual socioeconomic status or other factors.
The team has assessed racial/ethnic differences in diabetes treatment and disease outcome among a large cohort of pediatric participants in the T1D Exchange Clinic Registry. The T1D Exchange Clinic Registry includes the records of more than 26,000 individuals with type 1 diabetes (T1D), ranging from one year to 93 years, with the goal of aiding researchers in conducting exploratory analysis, developing projects and having access to participants for future clinical studies. Of these participants, 10,704 were aged less than 18 years and had type 1 diabetes for more than one year; the mean age of the group was 11.9 years and 48% were female. This pediatric group was studied in terms of diabetes management and outcome, taking into consideration individuals’ ethnicities. Within the group, 83% (8841) were non-Hispanic white (white), 7% (697) were non-Hispanic black (black), and 11% (1166) were Hispanic; within this population, 214 high-income black and Hispanic families were included.
The team found that after adjusting the results for age, gender, diabetes duration and socioeconomic status, insulin pump use was more frequent among white participants (61%) in comparison to black (26%) or Hispanic (39%). Insulin pumps are devices that deliver rapid- or short-acting insulin 24 hours a day through a catheter placed under the skin, maintaining blood glucose within proper levels between meals and overnight. Black participants were found to have higher use of hemoglobin A1c, which is a blood test that provides information about the average blood sugar control over the past 2 to 3 months. Black participants also experienced a higher number of diabetic ketoacidosis (where due to low insulin levels, the body starts burning fatty acids and producing acidic ketone bodies, resulting in dehydration, vomiting, gasping for breath and sometimes coma) and severe hypoglycemic (low blood glucose levels) events in comparison to Hispanic or white participants. Between white and Hispanic participants, no significant differences were observed in hemoglobin A1c, diabetic ketoacidosis, or severe hypoglycemia.
Researchers concluded that even after adjustment for children’s socioeconomic status, there were evident differences in the insulin delivery method and therapy outcome, especially in the ethnic group black versus the white and Hispanic. The team believes that future studies should explore the barriers around insulin pump use in the different ethnic groups as well as regarding optimal glycemic control, regardless of individual socioeconomic status.


