After living with diabetes for a while, you begin to realize that we actually have available several tools available in different shapes, colors and features to help us track Diabetes. In fact, there are so many different types of medical devices for diabetes management that you could almost compare the collection of devices we have available to us with that of a watch collector’s!
For instance, let’s look at glucose measurement devices: since I was first diagnosed I’ve had around 4 different devices. Each of them requires a specific type of supportive equipment. Then each doctor usually recommends a specific set of treatment, which might require the use of different insulin pens to inject each different type of insulin. The variety among these tools is amazing — even the needles used can vary in size, which can also directly influence treatment efficiency.
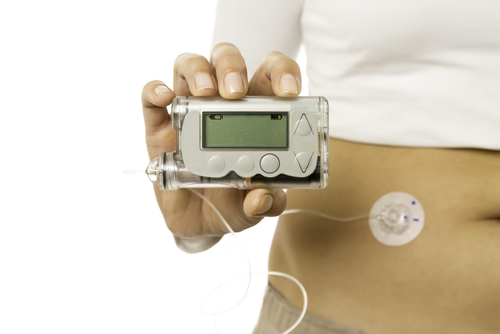
A quite recent device that many doctors recommend as offering better control of the disease are insulin pumps. Insulin Pumps are small computerized devices that allow insulin delivery in two ways: (1) in a basal way, mimicking the healthy human body, (2) and as a “bonus” dose, in reaction to punctual hyperglycaemia episodes.
 A pump is a continuous tracking system that is always connected to your body and gives a bit more autonomy to its users, since the pump itself can be programmed to inject a basal volume of insulin throughout the day and make “special deliveries” of insulin at specific times. Because the technology provides constant regulation, pumps generally offer a better control of glucose levels, and it is normal for pump users to experience a decrease in their level of A1C hemoglobyn. The main disadvantage of the device is the investment: since it is a “smart” tool, it is naturally more expensive than the traditional insulin pens.
A pump is a continuous tracking system that is always connected to your body and gives a bit more autonomy to its users, since the pump itself can be programmed to inject a basal volume of insulin throughout the day and make “special deliveries” of insulin at specific times. Because the technology provides constant regulation, pumps generally offer a better control of glucose levels, and it is normal for pump users to experience a decrease in their level of A1C hemoglobyn. The main disadvantage of the device is the investment: since it is a “smart” tool, it is naturally more expensive than the traditional insulin pens.
Personally, I have had the opportunity to use a pump, but because I play sports, I did not feel comfortable having to wear a device that is bigger than a belt hanging down over my belly. Nevertheless, this was a personal choice, which I am pretty sure that my doctors and family would have liked me to reconsider. The thing is, at the end of the day, we are the ones who have to feel comfortable with our own choices. If you have a pump but you don’t clean it or you leave the needle out of your system, it is your responsibility as a diabetic for not taking a proper care of the device. And the same applies to me and my traditional devices.
Something that has allowed me to adjust my glucose measurement habits was making a mental note of not going to the lunch/dinner table before knowing how much I can eat, and I only know this after measuring my glucose level. At first it was a bit weird to have to stop everything to make this measurement, but soon it became a golden habit.
If you want to know more about diabetes’ basics, take a look back at my first post.